Diabetes: Get to know the signs and symptoms
- Jul 3, 2013
- 4 min read
Updated: Feb 16, 2022
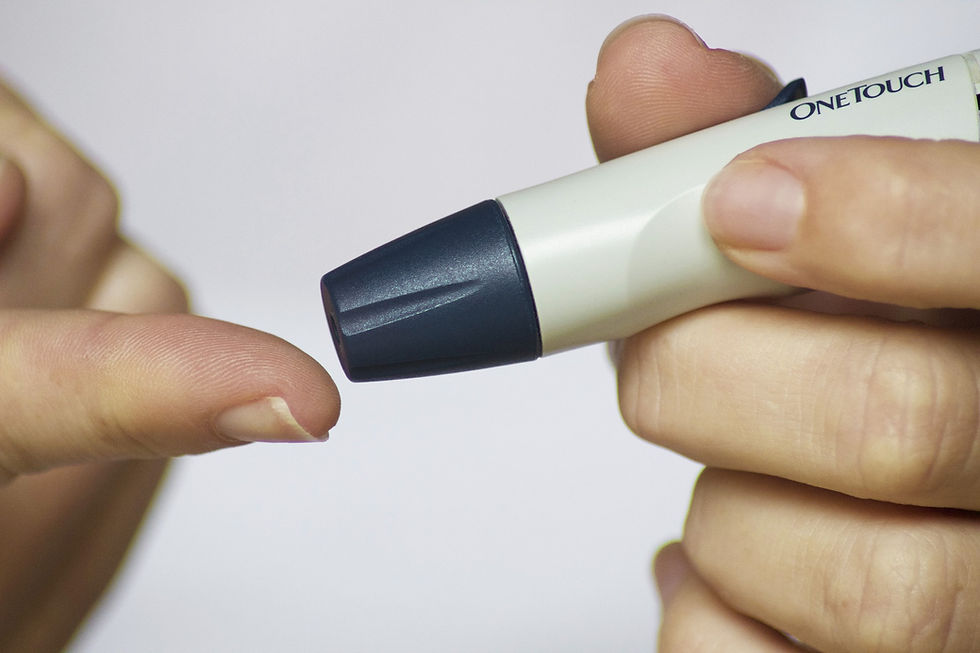
Approximately, 3 million people have diabetes in the UK, but may not yet have developed the symptoms. Diabetes is a long-term condition which can occur at any age, so it’s important that you get to know how to recognise the symptoms. For more information on Diabetes, please click here. For more information on the symptoms of Diabetes, please click here. Diabetes is linked to insulin, a hormone produced by the beta cells in the pancreas to aid the digestion of carbohydrates, being either absent or working ineffectively. Insulin gets the glucose into the cells for energy, so when insulin is absent or working ineffectively, glucose builds up instead in the bloodstream. Not everyone will have the symptoms, especially if their diabetes has developed very slowly over time, however even if so, the key signs and indicators to look out for include: tiredness, frequent urination, a quenching thirst, frequent urinary infections or thrush and also weight loss.
There are 2 types of diabetes which have very different causes:
Type 1 Diabetes
Around 10 – 15% of people in the UK have Type 1 diabetes, making it the less common form.
It’s caused by a complete lack of insulin, due to the beta cells in the pancreas being destroyed by the body’s own immune system. So because the destruction process is always ongoing people who have diabetes are more likely to develop the symptoms much quicker, such as becoming extremely unwell in the space of just a few weeks, with sudden dramatic weight loss and an unquenching thirst.
Type 1 diabetes is most commonly found in younger people, so it can appear during childhood or adolescence and sadly even in very young babies. But yet again it can be found to occur at any age.
Type 1 Diabetes treatment
Treatment is always with insulin via injection or an insulin pump. The treatment aims to try replace the insulin in a way which closely reflects how the body would naturally in a person who doesn’t have diabetes.
Insulin treatments today are much more sophisticated than in the last 20 years. Typically, people have 1 or 2 long acting injections and 3 or more quick acting injections each day. The reason for this is an attempt to try and mimic what the body would normally do.
Insulin pumps that are worn externally 24/7 are more sophisticated in giving insulin. Type 1 diabetes sufferers use quick acting insulin pumps, as they have a constant supply and can programme their pump to top up their insulin as and whenever they require it. Presently, insulin pumps are the most sophisticated method of insulin delivery and are mainly used for Type 1 diabetes.
Type 2 Diabetes
Type 2 diabetes accounts for approx. 90% of diabetes sufferers in the UK and is now very much seen as a killer disease because it also has strong links with the heart and circulatory disease.
Generally, people with Type 2 diabetes are still producing insulin at diagnosis of the condition, but are either not producing enough or they have 'insulin resistance', where insulin is present but the body cells are simply resistant to it.
Either way, in order to combat this, beta cells produce increasing amounts of insulin so are constantly overworking. This happens gradually over many, many years and so the diabetes condition may only get diagnosed once the blood glucose levels rise after the beta cells can no longer keep up.
Type 2 diabetes is a progressive condition and can sometimes be managed by sensible changes to the sufferer’s diet and lifestyle or via their medication. However, over 50% of people with Type 2 diabetes will need insulin injections within 10 years of their diagnosis.
Type 2 diabetes symptoms often include being overweight, having high blood pressure and high cholesterol or other blood fats. This is known as the 'metabolic syndrome'. To read more information on this, please click here.
Type 2 diabetes generally appears in the older generation, but that is not to say that younger people including children aren’t being diagnosed with the condition, which is being associated to inactivity and obesity as a cause.
Type 2 Diabetes treatment
There is now a range of non-insulin medications that do various things such as encouraging additional insulin production. Some inhibit the body's own production of glucose and some try to combat insulin resistance.
The complications of Diabetes
In the short term, balancing blood glucose levels can be quite difficult and low blood glucose, known as “hypoglycaemia”, can occur if there is too much insulin. Early symptoms of hypoglycaemia can include:
1. Sweating
2. Shaking
3. Tingling lips
For more information, please click here. Symptoms which occur when the brain is extremely short of glucose, can lead to unconsciousness if not treated as soon as possible and can include: 1. Confusion 2. Aggression 3. Lack of co-operation
High blood glucose levels can also cause difficulties in the short term, which cause symptoms similar to those at initial diagnosis. If someone with Type 1 diabetes becomes acutely short of insulin in their body, they may develop diabetic ketoacidosis, where the blood glucose is very high. If this happens, emergency hospital treatment is required immediately.
For more information on diabetic ketoacidosis, please click here.
Long term complications of Diabetes If someone with diabetes often suffers high blood glucose levels over a number of years then they are at risk of developing diabetic specific complications such as: 1. Eyes (diabetic retinopathy) – this condition causes damage to the small blood vessels in the retina. Annual screening can pick up early signs. As also, laser treatment can be used, and it is much rarer nowadays for people to become blind from the condition. For more information, please click here. 2. Feet (peripheral neuropathy) - damage to peripheral nerves that causes gradual loss of feeling, resulting potentially in foot ulcers and possible amputation. For more information, please click here. 3. Kidneys (nephropathy) - gradual reduction in kidney function that may lead to renal failure and will require dialysis or a transplant. For more information, please click here. 4. Autonomic neuropathy – this is damage to 'involuntary' nerves like automatic systems, particularly heart rate and digestion. This is less common, but one of the more difficult ones to live with. Erectile dysfunction is part of the spectrum of autonomic neuropathy. For more information, please click here. For more information about Diabetes please the Diabetes UK website by clicking here.









































Comments